Overview
In an effort to combat poor infant feeding practices, the CBC Health Services started a Nutrition Improvement Program (NIP) with the overall goal to improve on the nutritional status of clients receiving services in CBC Health units in Cameroon. This is accomplished through education, sensitization, counselling, and promotion of optimal breast feeding practices and consumption of local food sources. The CBCHS’ NIP has trained over 50 nutrition counsellors who operate in close to 20 CBCHS’ facilities providing nutritional counselling services to clients and patients identified in the health units with various conditions such as HIV, diabetes, obesity, anemia, gout, arthritis, hepatitis and general infant feeding. They also demonstrate procedures on preparing enriched infant food, feeding during illness for low weight babies, and follow up infants during Infant Welfare Clinic/Well Baby clinics.
Purpose
To improve the nutritional status of clients receiving services in the CBC health units in Cameroon.
Activities of the Program
Provide nutritional counselling services to clients and patients with various conditions e.g general infant feeding (prevention of breast engorgement, proper attachment/positioning to breast, nutritional support for PLWHA, nutrition and diabetes, nutrition and hypertension, diet and gouts, arthritis, overweight/obesity, anemia, constipation, gastritis, liver conditions (hepatitis) and medications.
Demonstrate the preparation of enriched infant foods, feeding during illness for low weight babies etc.
Access Points
The Nutrition counselling services are offered in the following CBC Health Services facilities: Mbingo, Banso, Mutengene, Mboppi, Kumba, Nkwen, Bonaberi, Etoug-Ebe, Ekoundoum, Nkoabang, Voundou, Ndu, Bafoussam, Banyo, Belo, Ngounso and Mbougham LAP.
The CBCHS NIP collaborates with the St. Mary Solidad Catholic Hospital in Bamenda in training and supervising their nutrition counselors.
Partnership
The CBCHS signed an MoU with Danone, an Infant Nutrition Company aimed at supporting NIP activities within the confines of its vision, mission and goal.
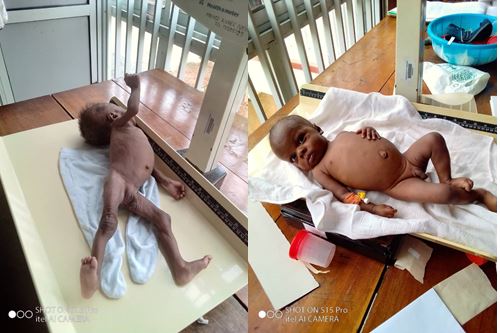
Titi on admission 7 months with weight 2.5kg. Discharge from Hospital weight 3.6kg
Testimonies of the Advantages of exclusive and prolonged Breast feeding
Silva (Pseudo name) is 37 years old and has 4 children. Her last child is 26 months. As a result of the nutrition counseling that she received immediately after delivery at maternity and in her subsequent visits for child’s vaccination, she decided to practice optimal breastfeeding for her fourth daughter where she breastfed for 28 months. Sylva testifies a significant difference between her fourth daughter and her other children. The child is stronger and very healthy, intelligent, smart and hardly consults in the hospital. Sylva says she likes to follow the nutrition counselor’s advice. She has one common challenge which is time as she has to take care of her other children and husband but to her the advantages of breastfeeding as explained to her by the nutrition counselor helps her to practice optimal breastfeeding. Sylva therefore plays advocate for the Nutrition Improvement Program.
